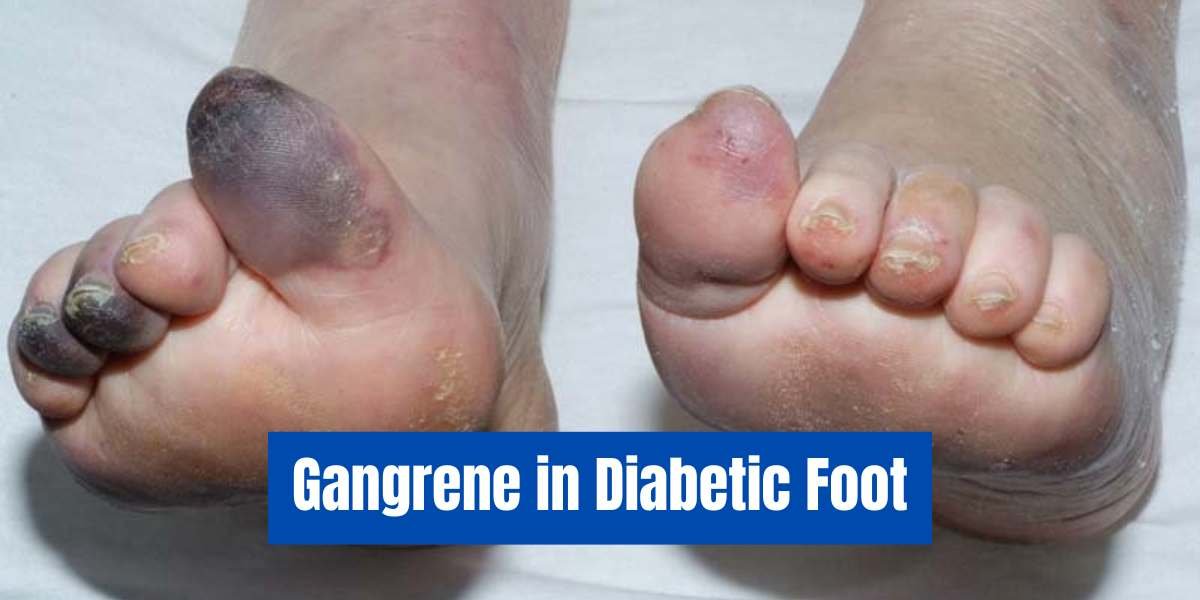
Gangrene in diabetic foot is a serious medical condition where body tissue dies due to a lack of blood supply or severe infection. People with diabetes are at a higher risk because high blood sugar levels can damage blood vessels and nerves over time. This reduces circulation and delays wound healing, making even small cuts dangerous.
In India, rising diabetes cases have led to an increase in diabetic foot complications, including gangrene. If not treated early, gangrene can progress rapidly and may result in amputation. The good news is that early detection and timely medical care can significantly improve outcomes and help save the affected limb.
What is Gangrene in Diabetic Foot?
Gangrene in diabetic foot occurs when tissue in the foot dies due to poor blood flow or infection. Diabetes plays a major role in this process:
- Poor blood circulation: High glucose levels damage blood vessels, reducing oxygen supply to tissues.
- Nerve damage (neuropathy): Loss of sensation means patients may not feel injuries or wounds.
- Slow wound healing: Even minor cuts or blisters can take longer to heal and become infected.
Types of Gangrene
Understanding the types of gangrene can help identify the severity of the condition:
- Dry Gangrene:
Common in diabetic patients, it occurs due to reduced blood flow. The skin becomes dry, shriveled, and dark. - Wet Gangrene: (neuropathy):
Caused by bacterial infection, this type spreads quickly and is a medical emergency. It often presents with swelling and discharge. - Gas Gangrene:
A rare but severe infection caused by bacteria producing gas within tissues. It progresses rapidly and requires urgent treatment.
Early Warning Signs of Gangrene in Diabetic Foot
Recognizing early symptoms of gangrene in diabetic foot can prevent serious complications. Watch out for:
- Skin color changes: The skin may turn from red to purple and eventually black.
- Swelling and blisters: Unusual swelling or fluid-filled blisters can indicate infection.
- Foul-smelling discharge: A strong odor from a wound is often a sign of tissue decay.
- Sudden pain or numbness: Some patients experience severe pain, while others may feel no sensation due to nerve damage.
- Cold, dry, or shiny skin: Reduced blood flow can make the skin appear tight, glossy, or unusually cold.
When to See a Doctor
Timely medical intervention can prevent complications and improve recovery. Consult a specialist if you notice:
- Wounds that are not healing within a few days
- Increasing pain, redness, or foul smell
- Signs of infection such as fever
- Blackened or discolored skin
Treatment Options Available
Treatment for gangrene in diabetic foot depends on the severity and stage of the condition. Common approaches include:
- Debridement: Removal of dead or infected tissue to promote healing
- Antibiotics: Used to control bacterial infection
- Advanced wound care: Includes specialized dressings and therapies to support healing
- Surgery: In severe cases, surgical intervention may be required to prevent the spread of infection
Early treatment significantly improves the chances of saving the foot and avoiding amputation.
Expert Care in Delhi
For effective management of gangrene in diabetic foot, consulting an experienced specialist is essential.
Dr. Anshumali Misra
- MCh - Plastic Surgery, MBBS, DNB - General Surgery
- 24+ Years Experience
Dr. Misra is highly regarded for providing advanced diabetic foot treatment in Delhi, with a strong focus on limb salvage and modern wound care techniques. His patient-centric approach and expertise make him a trusted diabetic foot doctor in Delhi for managing complex cases, including gangrene.
Prevention Tips
Preventing gangrene in diabetic foot starts with proper care and awareness:
- Inspect your feet daily for cuts, blisters, or discoloration
- Maintain good blood sugar control
- Wear comfortable, protective footwear
- Keep feet clean and moisturized
- Seek early treatment for any injury or infection
Conclusion
Gangrene in diabetic foot is a serious but preventable condition. Early warning signs like skin discoloration, foul odor, and non-healing wounds should never be ignored. With timely diagnosis and expert care, the risk of complications can be greatly reduced.